B 1/7 Mahanagar Extension ( Opp. Sahara India Centre ), Kapoorthala, Lucknow - 226006
Mon - Sat: 11:00am to 8:00pm
If you or a family member is living with diabetes, you know that keeping your blood sugar in check is a daily priority. You likely monitor your diet, take your prescribed medications, and visit your general physician regularly. However, there is one vital part of the body that many diabetic patients overlook until serious problems begin: the eyes.
Diabetes can quietly cause severe damage to your vision over time. The most common and dangerous eye condition associated with high blood sugar is called diabetic retinopathy. At Susanjeevani Hospital, our highly experienced eye specialist doctors in Lucknow, regularly treats patients who have suffered preventable vision loss simply because they were unaware of the risks or skipped their routine retina checkups.
This guide is designed to give you complete clarity on diabetic retinopathy. We will explain exactly what it is in simple terms, who is at the highest risk, how doctors diagnose it, the advanced treatment options available, and the practical steps you can take today to safeguard your sight.
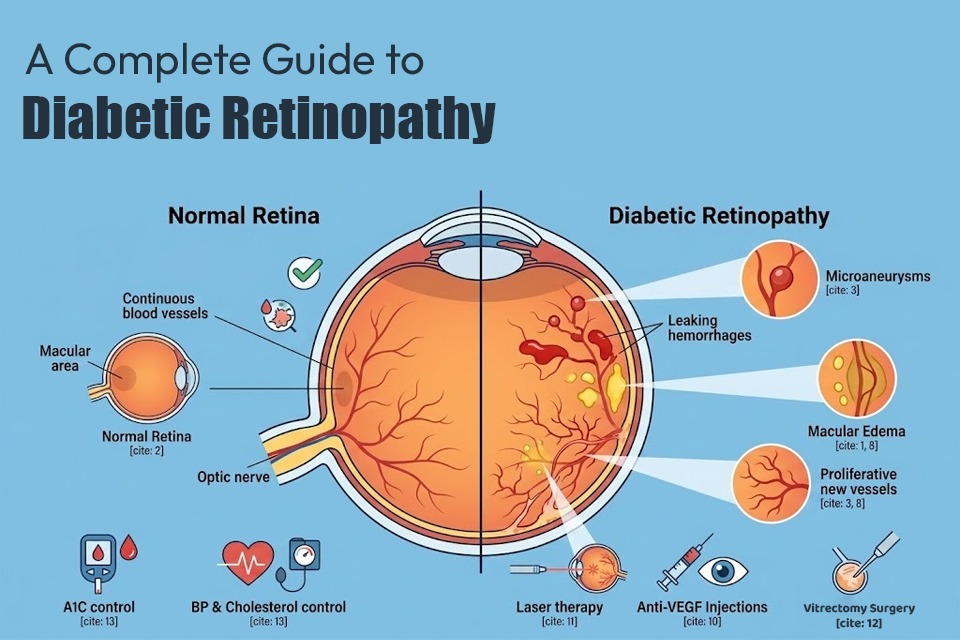
What is Diabetic Retinopathy?
To understand how diabetes harms your vision, you first need to understand a very important part of your eye called the retina. The retina is the light-sensitive layer of nerve tissue located at the very back of the inside of your eye. You can think of it like the film inside a traditional camera. When light enters your eye, it hits the retina, which then sends visual signals to your brain through the optic nerve. This process is what allows you to see the world around you.
Diabetic retinopathy is a medical condition where chronically high blood sugar levels cause direct damage to the tiny, delicate blood vessels that nourish the retina.
When your blood sugar stays too high for a long period, it damages the walls of these small blood vessels. This damage causes the vessels to become blocked, cutting off the vital blood and oxygen supply to the retina. In response to this starvation, the eye attempts to fix the problem by growing entirely new blood vessels. Unfortunately, these new blood vessels do not grow properly. They are extremely fragile, weak, and prone to leaking blood and fluid directly into the eye.
This leakage causes severe swelling, damages the sensitive retinal tissue, and can eventually lead to permanent vision loss or total blindness if left untreated by a specialist.
Understanding Diabetic Macular Edema (DME)
Often, diabetic retinopathy is accompanied by a secondary condition known as Diabetic Macular Edema (DME). The macula is the small, highly sensitive central area of the retina. It is responsible for your sharp, straight-ahead vision—the vision you rely on to read a book, drive a car, or recognize a loved one's face
When the damaged retinal blood vessels leak fluid, that fluid can build up in the macula. This causes the macula to swell like a sponge (edema). When the macula swells, your central vision becomes blurry, washed out, and distorted.
The 4 Stages of Diabetic Eye Disease
Diabetic retinopathy does not cause blindness overnight. It is a progressive disease that develops slowly through four distinct stages. Understanding these stages is critical because detecting the disease early can literally save your sight.
1. Mild Nonproliferative Diabetic Retinopathy (NPDR)
This is the earliest and mildest stage of the disease. At this point, tiny balloon-like bulges called microaneurysms begin to appear in the walls of the small blood vessels of the retina. These weak spots may leak tiny amounts of blood or fluid into the retinal tissue. During this early stage, patients almost never notice any changes in their vision, which is why regular eye exams are so crucial.
2. Moderate Nonproliferative Diabetic Retinopathy (NPDR)
As diabetes continues to affect the body, the disease progresses to the moderate stage. Here, some of the blood vessels that nourish the retina become swollen and completely blocked. This blockage reduces the necessary blood supply to the retina. The physical swelling can also start to affect the macula, increasing the patient's risk of developing Diabetic Macular Edema.
3. Severe Nonproliferative Diabetic Retinopathy (NPDR)
In this advanced stage, a significant number of retinal blood vessels become blocked, severely starving the retina of its blood and oxygen supply. Because the retina is suffocating, it starts sending out desperate chemical signals to the body, demanding the growth of new blood vessels to replace the blocked ones.
4. Proliferative Diabetic Retinopathy (PDR)
This is the final, most advanced, and most dangerous stage of diabetic eye disease. Prompted by the chemical signals from the starving retina, new, abnormal blood vessels begin to grow (proliferate) along the inside surface of the retina and into the vitreous gel. The vitreous is the clear, jelly-like substance that fills the center of your eye.
Because these new blood vessels are abnormal and incredibly fragile, they can easily break and bleed heavily into the vitreous gel. This bleeding can completely block light from reaching the retina, causing sudden and severe vision loss. Furthermore, the growth of these new vessels brings along scar tissue. As this scar tissue naturally shrinks over time, it pulls on the retina. This pulling can cause the retina to detach from the back of the eye—a severe medical emergency known as a retinal detachment, which can lead to permanent blindness without immediate surgery.
What Are the Symptoms of Diabetic Retinopathy?
One of the most dangerous characteristics of diabetic retinopathy is that it is a "silent" disease in its early stages. You can have early or even moderate retina damage and still have perfect, painless vision.
However, as the condition worsens into the severe and proliferative stages, or if macular edema develops, you may start to experience the following warning signs:
- Floaters: Seeing dark spots, dots, or cobweb-like strings floating across your vision. This is often the first sign of bleeding inside the eye.
- Blurred Vision: Objects at a distance or up close may look fuzzy or out of focus.
- Fluctuating Vision: Your ability to see clearly might change from day to day, or even from morning to night, depending on your blood sugar levels.
- Washed-out Colors: Colors might look faded, dull, or difficult to distinguish.
- Dark or Empty Areas: You may notice blind spots, shadows, or a dark curtain appearing in your field of view.
- Sudden Vision Loss: Complete or partial loss of vision that happens very quickly requires immediate emergency medical attention.
If you have diabetes and notice any of these symptoms, do not wait to see if they get better. Contact Susanjeevani Hospital immediately for an urgent consultation.
Who is at High Risk?
Anyone diagnosed with type 1 diabetes, type 2 diabetes, or gestational diabetes (diabetes during pregnancy) is at risk of developing diabetic retinopathy. However, certain medical and lifestyle factors greatly increase your chances of developing the condition or causing it to progress much faster:
- Duration of Diabetes: This is the biggest risk factor. The longer you have lived with diabetes, the higher your risk of developing retinopathy.
- Poor Blood Sugar Control: Consistently high blood sugar levels over months and years cause the most severe damage to the retinal blood vessels.
- High Blood Pressure (Hypertension): High blood pressure damages blood vessels throughout your entire body. When combined with diabetes, it puts extreme strain on the delicate vessels in your eyes.
- High Cholesterol: Extra fat and lipids in your blood can build up inside the blood vessels, leading to faster blockages and leakage.
- Pregnancy: Women who develop gestational diabetes, or women who already have diabetes and become pregnant, face a significantly higher risk of rapid eye damage.
- Tobacco Use: Smoking narrows all blood vessels and drastically increases the risk of severe diabetic complications, including irreversible eye damage.
How Do We Diagnose Diabetic Eye Damage?
You cannot self-diagnose diabetic retinopathy, and simply getting a new prescription for reading glasses will not detect the disease. The only way to accurately diagnose this condition is through a comprehensive, dilated eye exam performed by an eye specialist.
At Susanjeevani Hospital, Dr. Mohit Khemchandani uses highly advanced diagnostic technology to evaluate the health of your retina:
Dilated Eye Exam
The doctor will place special drops in your eyes to widen (dilate) your pupils. This acts like opening a window, allowing the doctor to look deep inside the eye with a special magnifying lens. They will carefully check for swollen blood vessels, microscopic leaks, scar tissue, and any changes to the optic nerve.
Optical Coherence Tomography (OCT)
This is a quick, completely painless imaging test that uses safe light waves to take highly detailed cross-section pictures of your retina. An OCT scan allows the doctor to measure the exact thickness of your retina and detect even the tiniest amount of fluid swelling in the macula.
Fluorescein Angiography
If severe damage or abnormal blood vessels are suspected, this specialized test is performed. A yellow, vegetable-based dye is injected into a vein in your arm. As the dye travels through your bloodstream and into the blood vessels of your eyes, a special camera takes rapid photographs. This test creates a precise map, highlighting exactly which blood vessels are blocked, leaking, or growing abnormally.
Diabetic Retinopathy Treatment in Lucknow
If you are diagnosed with diabetic eye disease, your treatment plan will depend entirely on the stage of the disease and whether or not your macula is swollen. The primary goal of all treatments is to stop or slow down the progression of vision loss. It is important for patients to understand that while treatments are highly effective, they do not cure diabetes itself.
As a leading Vitreo Retina Specialist, Dr. Mohit Khemchandani offers comprehensive diabetic retinopathy treatment in Lucknow, utilizing the latest medical advancements:
1. Medical Management and Observation
If you are diagnosed with mild or moderate nonproliferative diabetic retinopathy and do not have macular edema, you may not need any eye injections or surgery right away. Instead, the immediate treatment is strict medical management. You will need to work closely with your physician to gain tight control over your blood sugar, blood pressure, and cholesterol. Dr. Khemchandani will monitor your eyes very closely every few months to ensure the condition is not advancing.
2. Anti-VEGF Eye Injections
When the eye starts growing abnormal, leaky blood vessels, it does so by producing a specific protein called VEGF (vascular endothelial growth factor). Anti-VEGF medications are injected directly into the eye to block this protein. This highly effective treatment stops the growth of new blood vessels and quickly reduces swelling in the macula. While the thought of an eye injection can be intimidating, the eye is thoroughly numbed with anesthetic drops beforehand, and most patients experience little to no discomfort.
3. Laser Therapy (Focal/Grid Laser)
This specific type of laser treatment is designed to treat Diabetic Macular Edema. The doctor uses a highly focused, microscopic laser to gently burn and seal off the specific leaking blood vessels in the center of the retina. This stops fluid from building up and reduces the swelling in the macula, helping to protect and stabilize your central reading vision.
4. Panretinal Photocoagulation (Scatter Laser Treatment)
This aggressive laser treatment is used for patients in the advanced, proliferative stage of the disease. The doctor uses a laser to create hundreds of tiny, scattered burns in the peripheral (outer) areas of the retina. This process intentionally shrinks the abnormal new blood vessels and stops them from growing further. It is a highly effective way to reduce the risk of severe bleeding into the eye and prevent retinal detachment.
5. Vitrectomy Surgery
If your condition has reached a very advanced stage—meaning there is a massive amount of blood in the vitreous gel that is blinding you and will not clear on its own, or if thick scar tissue is pulling the retina away from the wall of the eye—a surgical procedure called a vitrectomy is required. During this delicate microsurgery, Dr. Mohit Khemchandani makes tiny, keyhole incisions in the eye to carefully remove the blood-filled vitreous gel and peel away the dangerous scar tissue. The gel is then replaced with a clear medical solution, a gas bubble, or silicone oil to push the retina back into its proper, healthy position.
How to Prevent Diabetic Eye Disease
The absolute best treatment for diabetic retinopathy is preventing it from ever developing in the first place. As a diabetic patient, you have a massive amount of control over your long-term eye health. Here are the most effective steps you can take to prevent vision loss:
- Control Your Blood Sugar (A1C): Work with your doctor to keep your HbA1c levels within your target range. Consistent blood sugar control is your strongest shield against retinal damage.
- Manage Blood Pressure and Cholesterol: Keep your blood pressure and cholesterol levels in a healthy range to reduce the strain on your eye's blood vessels.
- Never Skip Your Annual Retina Exam: If you have diabetes, you must undergo a comprehensive dilated eye exam at least once a year, even if your vision feels perfect. Early detection is the only way to stop the disease before it causes blindness.
- Adopt a Diabetic-Friendly Diet: Eat a balanced diet rich in leafy green vegetables, whole grains, and lean proteins. Strictly avoid sugary drinks, sweets, and highly processed carbohydrates that cause rapid spikes in your blood sugar.
- Stay Physically Active: Regular exercise helps your body use insulin more effectively. Aim for at least 30 to 40 minutes of brisk walking or moderate exercise every day.
- Quit Smoking Immediately: Smoking accelerates diabetic damage to your blood vessels faster than almost anything else. Quitting is essential for preserving your vision.
Frequently Asked Questions (FAQs)
1. Can diabetic retinopathy be cured completely?
2. Does diabetic retinopathy always cause blindness?
3. Will changing my glasses prescription fix the blurry vision caused by diabetes?
4. Is laser treatment for diabetic retinopathy painful?
5. How often should I get my eyes checked if I have diabetes?
Book Your Retina Checkup at Susanjeevani Hospital
Living with diabetes means you have to be proactive about your health, but it does not mean you are destined to lose your vision. By controlling your blood sugar and partnering with a trusted eye specialist, you can enjoy clear sight for your entire life.
Do not wait for your vision to become blurry or for dark spots to appear. If you are diabetic and have not had a comprehensive retina evaluation in the past year, you need to take action today.
At Susanjeevani Hospital, our dedicated eye care team is fully equipped with state-of-the-art diagnostic imaging and advanced surgical technology. Dr. Mohit Khemchandani , our highly experienced Vitreo Retina Specialist, is dedicated to providing thorough, medically accurate, and compassionate care to protect your vision.
Contact Us to Schedule Your Appointment Today:
📍 Address: B 1/7, opp. Sahara India Centre, Mahanagar Extension, Kapoorthala, Lucknow, Uttar Pradesh 226006
📞 Phone: 84008 68388
